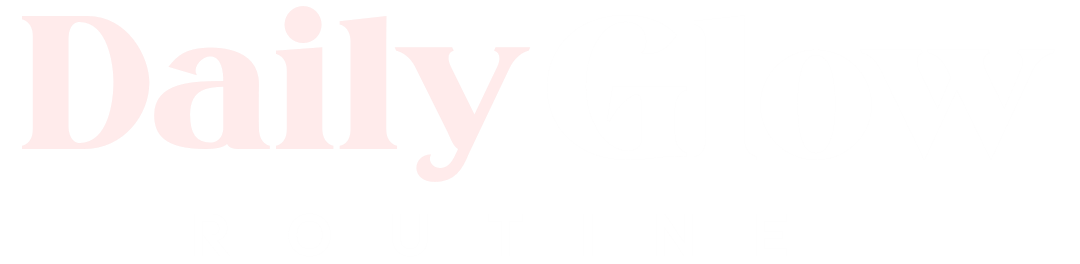Stopping steroids can trigger an acne flare on the chest and back (sometimes called “steroid rebound” or steroid-induced acne). That’s frustrating — especially for guys who train hard, wear backpacks, or want to feel confident shirtless — but most cases are manageable with gentle habits, targeted topical care, and the right hygiene. Below is a practical, step-by-step guide that covers what to expect, how to treat breakouts safely at home, when to see a dermatologist, and how to avoid making things worse while your skin calms down.
Important: if you’re under 18, talk to a parent/guardian and your doctor before starting any new topical medication or if your acne is severe. This guide gives safe, non-prescription-friendly steps plus pointers on when to get professional help.
Why Acne Can Flare After Stopping Steroids
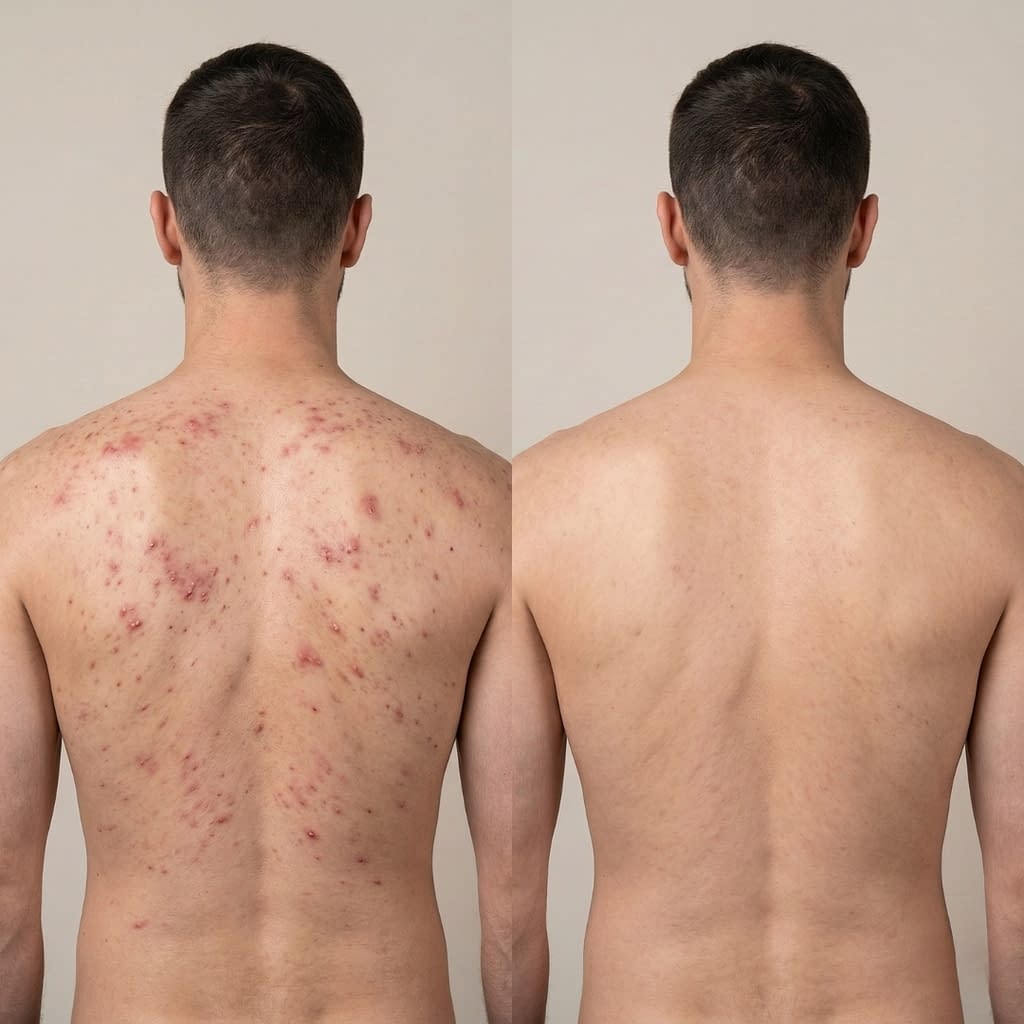
When you stop systemic or topical steroids, your hormones and immune responses can rebalance suddenly. Steroids often suppress inflammation and immune activity; when they’re removed, inflammation can rebound and oil production or follicular inflammation can increase — producing a sudden, sometimes intense acne flare. Additionally, steroids can cause follicular keratinization (pores getting clogged) which shows up as multiple similar bumps clustered on the back and chest.
The good news: steroid-related flares are usually temporary but may take weeks to months to fully settle. With the right steps you can speed recovery and reduce the risk of scarring.
Steroid-Induced Acne vs. Regular Acne: Know the Difference
Understanding the type helps you treat it appropriately.
- Steroid-induced acne
- Often appears suddenly after starting or stopping steroids.
- Lesions can be numerous, appear similar in size, and concentrate on the chest, upper back, and shoulders.
- Can include inflammatory papules and pustules; sometimes nodules appear.
- Regular (acne vulgaris)
- Often linked to puberty, hormones, genetics, or blocked follicles.
- Typically includes a mix of comedones (blackheads/whiteheads), papules, pustules, and sometimes cysts.
If your flare started right after a steroid course or after stopping a steroid medication, treat it as steroid-related and be extra cautious with aggressive DIY fixes.
Typical Timeline: What to Expect After You Stop
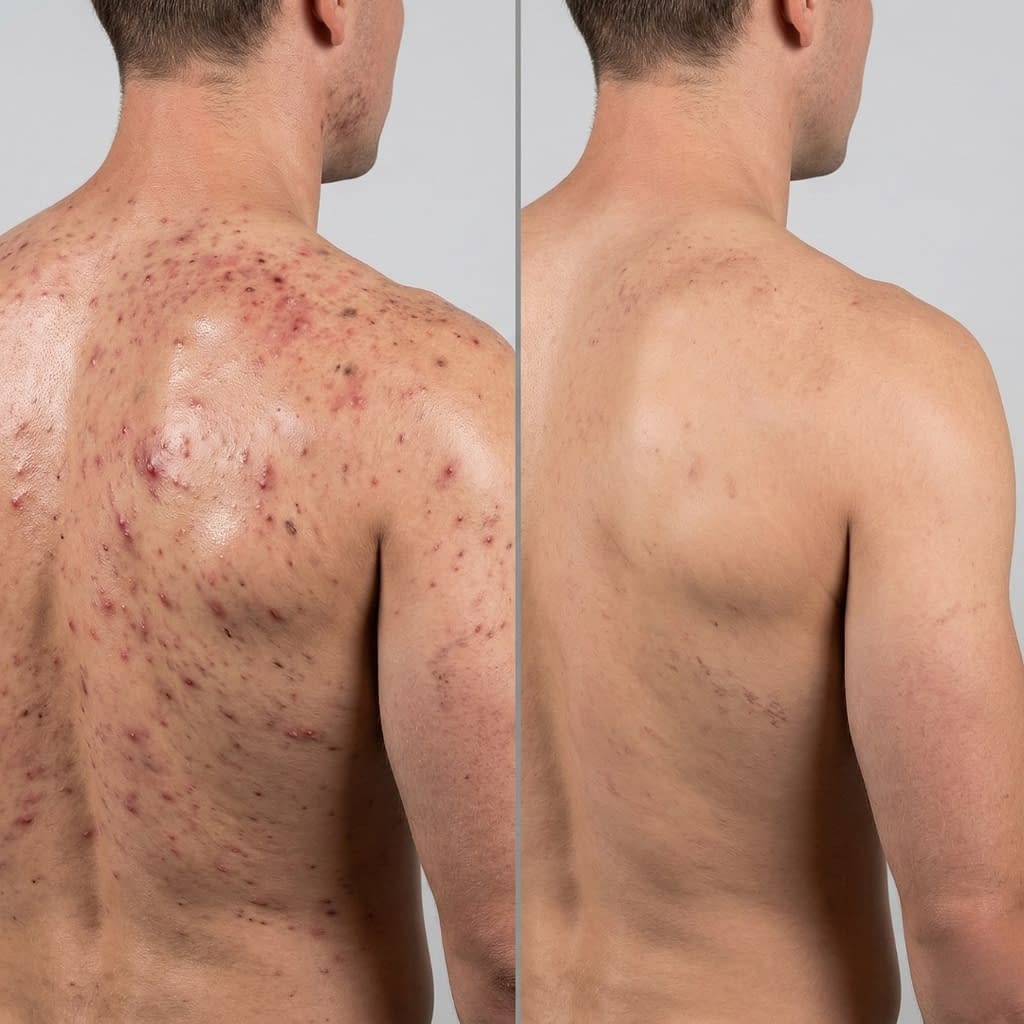
- Days–2 weeks: acne may appear or worsen; new inflamed bumps show up.
- 2–8 weeks: the worst of the flare often peaks and then gradually eases as hormones and immune responses recalibrate.
- 8+ weeks: many people see steady improvement; persistent deep nodules or scars need professional care.
Patience is essential — treatment plus consistent habits typically yields visible improvement in 4–12 weeks.
How to Identify Severity: Mild, Moderate, or Severe Breakouts
Quick self-check:
- Mild: a few inflamed bumps and isolated pustules across the back.
- Moderate: many inflamed papules/pustules covering parts of the back; occasional painful bumps.
- Severe: widespread, painful nodules or cysts, grouped clusters, or early scarring.
If you have severe nodules/cysts, spreading infection (increasing pain, warmth, fever, or pus), or early scarring, see a dermatologist sooner rather than later.
Gentle Cleansing and Shower Habits That Help
Good shower and cleansing habits are the foundation.
Step-by-step shower routine
- Shower after sweating (gym, hot weather) — sweat trapped on skin promotes bacteria and worsens inflammation.
- Use a gentle, targeted body cleanser with acne-friendly ingredients (benzoyl peroxide body washes or salicylic-acid washes — see next section). Avoid harsh, grainy scrubs that irritate skin.
- Wash the back with a long-handled soft bristle brush or a microfiber cloth to reach the area without aggressive scrubbing. Use light pressure; don’t rub raw skin.
- Rinse thoroughly with lukewarm water — hot water can increase irritation.
- Pat dry with a clean towel. Don’t rub — friction spreads bacteria and inflames follicles.
- Apply topical products (see treatments) to slightly damp skin for better absorption.
Frequency: once daily is usually fine; if you sweat a lot or after workouts, rinse afterward with water or your body wash.
Exfoliation for the Back: Safe Use of BHAs and Physical Methods
Chemical exfoliation is safer and more even than rough physical scrubs.
How to exfoliate safely
- Use a leave-on BHA (salicylic acid) product formulated for the body (0.5–2% salicylic acid). BHAs penetrate oil and unclog pores gently. Apply 2–3 times weekly to start, then increase to nightly if tolerated.
- Avoid harsh physical scrubs while inflamed. If you use a physical exfoliant, choose a very gentle one and limit to once weekly, avoiding active pustules.
- Patch test first on a small area of your back for 24–48 hours to check for irritation.
- Pair exfoliation with soothing and hydrating care — BHAs can dry skin, so apply a lightweight, non-comedogenic moisturizer afterward.
BHAs are especially helpful on the back because they’re oil-soluble and get inside clogged follicles where benzoyl peroxide may not reach as well.
Topical Treatments That Work: Benzoyl Peroxide, Adapalene, and More
Topical, over-the-counter actives are effective for many back flares.
Safe topical options & how to use them
- Benzoyl peroxide (BPO) (2.5–5% cleansers or leave-on gels) — antibacterial and anti-inflammatory. Good for inflammatory pimples. Use as a wash or leave-on gel. Start at lower strength to reduce irritation. Apply once daily and increase if tolerated.
- Adapalene 0.1% gel (a retinoid) — helps normalize follicle turnover and prevent new clogged pores; available OTC in many places. Use at night, start every 2–3 nights to build tolerance, and increase to nightly as tolerated. Apply a thin layer to affected areas. (If you are under 18, check with a parent/guardian and doctor.)
- Salicylic acid (0.5–2%) — as a leave-on product or body wash, helps exfoliate and clear pores. Use 2–3× weekly initially.
- Combination approach: many people alternate BPO (morning) and adapalene (night) once skin tolerates both — this tackles bacteria and clogged follicles from both angles. Start slowly and patch-test.
- Spot treatments: sulfur or benzoyl peroxide spot gels can reduce inflammation quickly.
Important cautions:
- Don’t layer multiple strong actives at once — introduce one product at a time.
- Apply topicals to clean, dry skin and use a light moisturizer over if dryness occurs.
- If you experience severe irritation (redness, burning, widespread peeling), reduce frequency or stop and seek advice.
Spot Treatments and Soothing Ingredients to Reduce Inflammation

Calming inflamed lesions reduces pain and the chance of scarring.
Soothing options
- Niacinamide (2–5%) — topical serum or body lotion that reduces inflammation and helps barrier repair. Apply to the whole back as tolerated.
- Aloe vera gel or colloidal oatmeal products — soothe itching and redness.
- Low-strength topical hydrocortisone (1%) is sometimes used briefly to calm extreme irritation but should be discussed with a healthcare provider (avoid long-term steroid use).
- Cold compresses can relieve painful inflamed bumps briefly.
Spot treatment routine
- For a painful pustule, gently clean the area.
- Apply a small amount of benzoyl peroxide gel or a sulfur spot treatment.
- If the lesion is very red and hot, use a cool compress for 5–10 minutes and consult a clinician if it worsens or if you have systemic symptoms.
Avoid picking or squeezing — picking increases the risk of scarring and infection.
Clothing, Fabric, and Friction: How to Minimize Irritation
What you wear matters a lot for back acne.
Clothing tips
- Choose breathable, moisture-wicking fabrics (polyester blends, merino wool for outdoors, technical gym fabrics) that pull sweat away from skin. Cotton traps moisture.
- Wear loose-fitting shirts when you’re healing — tight clothing and backpacks create friction (acne mechanica).
- Change sweaty clothes quickly after workouts; don’t sit in sweaty shirts for long.
- Wash workout gear frequently and avoid heavy fabric softeners or fragranced detergents that can irritate skin.
- If you wear backpacks, try to reduce pressure or use a pack with ventilated straps; keep the contact area clean.
Reducing friction and moisture reduces new irritation and lets topical treatments work.
Gym and Hygiene Habits to Prevent Reinfestation and Worsening
Small gym habits prevent acne from cycling.
Gym hygiene checklist
- Shower after workouts using your acne-friendly wash.
- Use a clean towel — don’t reuse sweat-soaked towels.
- Wipe down equipment before use and after (to avoid transferring oils/bacteria).
- Avoid sitting shirtless on gym benches or place a clean towel between you and equipment.
- Shower gels: use your BPO or salicylic acid body wash in the shower after workouts (not every shower initially if it irritates — start with post-workout only).
Good gym hygiene makes a big difference for the back area.
Avoiding Pore-Clogging Body Products and Heavy Oils
What you put on your body matters.
Product rules
- Choose non-comedogenic body lotions labeled “non-comedogenic” or “won’t clog pores.”
- Avoid heavy oil-based balms and coconut oil on the back if you’re acne-prone — they can trap bacteria and minerals and worsen breakouts.
- Check labels: ingredients like isopropyl myristate, cocoa butter, or some heavy silicones may be pore-clogging for some people.
- Fragrance-free options are less likely to irritate inflamed skin.
If you need hydration after using drying acne products, use a light lotion with glycerin, ceramides, or squalane
When Diet, Sleep, and Stress Management Can Help
Lifestyle matters — they influence inflammation and healing.
Practical habits
- Sleep: aim for consistent, good-quality sleep — repair happens at night.
- Diet: a balanced diet with plenty of whole foods, vegetables, lean protein, and healthy fats supports healing. Some people notice benefits from reducing high-glycemic foods, dairy, or excessive sugar — experiment mindfully and track changes.
- Stress management: stress increases inflammation; simple practices like walk breaks, breathing exercises, or short workouts help reduce flare intensity.
- Hydration: drink water throughout the day to help overall skin health.
Lifestyle tweaks support topical treatments and speed recovery.
Treating Post-Acne Marks and Early Scarring on the Back
Hyperpigmentation and shallow scarring can follow acne — treat gently.
What to use for marks (not deep scars)
- Niacinamide and azelaic acid — both reduce pigmentation and inflammation, suitable for body application.
- Alpha hydroxy acids (AHAs) like lactic acid — mild chemical exfoliation can even skin tone; use cautiously and start weekly.
- Sunscreen or protective clothing — UV exposure darkens post-inflammatory marks; cover the back when possible or use UPF clothing. Applying sunscreen on the back is awkward — lightweight mineral or spray SPFs can help if skin is exposed.
- Professional options: for persistent marks or early rolling scars, dermatologists can offer microneedling, superficial peels, or targeted treatments — see a pro if marks persist after several months.
If you see indentations or deep scarring forming, consult a dermatologist early — treatments are more effective when started sooner.
When to See a Dermatologist: Signs You Need Professional Care
Get professional help if any of these apply:
- Widespread painful nodules or cysts that don’t respond in 2–4 weeks of conservative care.
- Rapidly worsening infection (increasing pain, spreading redness, fever, pus).
- Evidence of scarring or deep lesions forming.
- Topical care not helping after 8–12 weeks and lesions persist or are extensive.
- You want prescription options (topical antibiotics, oral antibiotics, hormonal therapy, or isotretinoin) — a dermatologist can tailor therapy and monitor safety.
- If you took systemic steroids recently and have severe acne, your clinician can coordinate care and ensure you’re supported safely.
A dermatologist can use stronger, faster treatments and professional procedures while minimizing scarring risk.
Long-Term Prevention: Building a Back-Acne-Friendly Routine

A simple routined plan you can stick with.
Daily / weekly routine
- Daily: shower after workouts, gentle cleanse with salicylic-acid or benzoyl-peroxide wash as needed; pat dry; apply non-comedogenic moisturizer or niacinamide lotion if skin feels dry.
- 2–3× weekly: leave-on salicylic acid or product with BHA (if tolerated).
- Weekly: deep-conditioning or moisturizing mask if skin is dry from acne products.
- Monthly: evaluate progress; if lesions persist, step up with dermatologist help.
Stick to one new treatment at a time and give 6–8 weeks to judge improvement.
Final Words
Back acne after stopping steroids is often temporary and very treatable. The most effective approach combines good hygiene (shower after sweat, breathable clothing), targeted topicals (benzoyl peroxide, salicylic acid, and adapalene introduced slowly), gentler exfoliation, and lifestyle supports (sleep, stress, diet). Avoid picking, heavy oils, and abrasive scrubs that make things worse. If you have severe nodules, early scarring, infection, or no improvement after a couple months, see a dermatologist who can prescribe stronger or systemic treatments and protect your skin from permanent scarring